In a series of posts giving a frank account of experiences on the NHS frontline, Sally Williams hears from Rosie Tasker, a critical care nurse at Cambridge University Hospitals NHS Foundation Trust. Whilst isolating at home like so many, Rosie is leading a new Relatives Communications Team. This is what she said on 19 May 2020.
It is extremely hard to tell a relative of someone who is critically ill with COVID-19 that they cannot visit their loved one in hospital. This has been upsetting for patients and their relatives, and emotionally draining for staff. The reason we’ve had to stop relatives from visiting critical care is to protect patients, their families and staff from further spread of the coronavirus.
This is the first time I can recall such restrictions being placed on visitors and we’ve worried about the impact it might have. We know that communication is vital to the wellbeing of patients and their relatives.
One of the ICU consultants, Dr Rowan Burnstein, had the idea of ensuring every patient in critical care at Addenbrooke’s Hospital has access to an iPad so that virtual meetings could be set up between families and loved ones using Skype.
Relatives Communications Team
Doctors and nurses in critical care are working under immense pressure to care for COVID-19 patients, so we didn’t want to absorb their time with trying to make Skype work. Families can also need support using technology to communicate with their relative. So, this led us to set up the Relatives Communications Team.
I was massively disappointed when, in March, the occupational health team at the hospital said that I had to isolate at home. I wanted to support colleagues during what was set to be a really difficult time. The first thing I did was register my home computer with the hospital’s bring your own device policy. This allowed me to access the hospital’s secure networks from home. I then recruited three other nurses and one healthcare assistant, who were also isolating at home, to join the new team. There are also chaplains and psychologists available to offer support to families.
When a patient is admitted we ask for an email address for their relative and send them information on a range of topics, including: frequently asked questions about intensive care; COVID-19; how relatives can look after themselves at this stressful time; and a guide on Skype. We also provide details of the hospital’s Patient Advice and Liaison Service (PALS), which invites relatives to email messages and photographs that staff then print off to share with their loved ones.
A typical day
Every day, each member of the team is assigned to one of the four critical care units at Addenbrooke’s Hospital. We go through the patient list to identify patients for whom a call would help. We look at the patient’s notes to see if their relatives have received an update or might need support. We note where relatives have called the unit to enquire about their loved one, including where they’ve said they really want to visit the patient. We then get in touch to see whether they would like us to facilitate a video call.
I hold the Relatives Communications Team phone. Doctors and nurses within the hospital can call this to request help in setting up a video call for a patient. Relatives can also call the phone to make their own request. My job is to liaise with the hospital team to agree a good time for the video call to happen.
We also do test run video calls with the relative, to make sure that their computer is running smoothly. I’m not the most tech savvy person, so I’ve had to learn new skills in order to help families who have never used a computer before. I’ve talked them through how to set up email and also Skype. We are exploring how to offer more help to people who don’t have access to a computer.
The impact of video calls
A video call is not the same as seeing your loved one face to face, but our hope is that it makes the whole experience a little easier. Some families have used the service to share the moment their loved one turned the corner; others have used it to say their final goodbyes.
We have definitely seen a positive impact of video calling for some patients. All the doctors and nurses are wearing full PPE, and that can be scary for patients. To see a familiar face, even through a computer screen, and hear a familiar voice, has been really comforting for patients who are often quite confused and stressed. For example, by facilitating a daily video call between one patient and his family, we have found that it has really helped this patient to settle in the afternoons.
Some relatives can find it hard to hear what is being said by bedside staff because of their masks. I sometimes join the video call to help explain what doctors and nurses are saying. Many relatives have found the video call enormously helpful. There are some who have found it distressing, which is useful feedback for us so that we know to provide extra support.
It is up to families whether they want children to participate in the video call. It can be helpful for children to see their relative and the surroundings they are in. However, one family turned the video off so that the child could talk to his dad in critical care without becoming distressed at seeing him. It’s not an easy situation and we wish families could visit their relative, so it’s about supporting them in the best way we can.
I recently received a call from a patient’s relative to say thank you for setting up a video call. She said it had improved her day by helping her feel less stressed. Knowing the service is making a positive impact is what gets me through self-isolation. The whole team has been so amazing in how they have come together.
We will continue to take this work forward and use these approaches in non-COVID settings. It’s been such a privilege to help patients and their relatives in this way, whilst also supporting the hospital team.
As told to Sally Williams
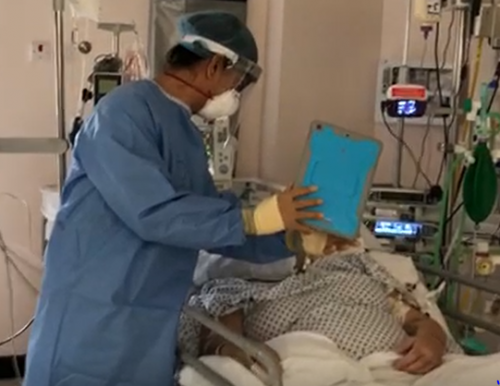
Image: a doctor at Addenbrooke’s Hospital holds up an iPad during a video call between a patient and their relative